Blood Glucose Meter Reimbursement
This topic is intended for Independent pharmacies only and is not applicable to Rexall pharmacies.
Various manufacturers offer online reimbursement for blood glucose meter warranty programs, and in some cases, lancets.
Select the appropriate tab to learn about reimbursement from the corresponding manufacturer.
Abbott Reimbursement Program
The Abbott Reimbursement Program is a drug plan available to all stores and patients for reimbursement of eligible blood glucose monitoring devices. The plan is adjudicated through TELUS Health Assure.
Abbott Meter and Lancet PINs
In Propel Rx, pseudo PINs were entered for each Abbott meter and lancet. To locate these PINs, search by trade name (e.g., FreeStyle Lite Meter, FreeStyle Lancets, etc.).
Patient Eligibility
To submit a claim to the reimbursement program for a meter or lancets, the following Third Party information must be added to the patient's Third Party tab.
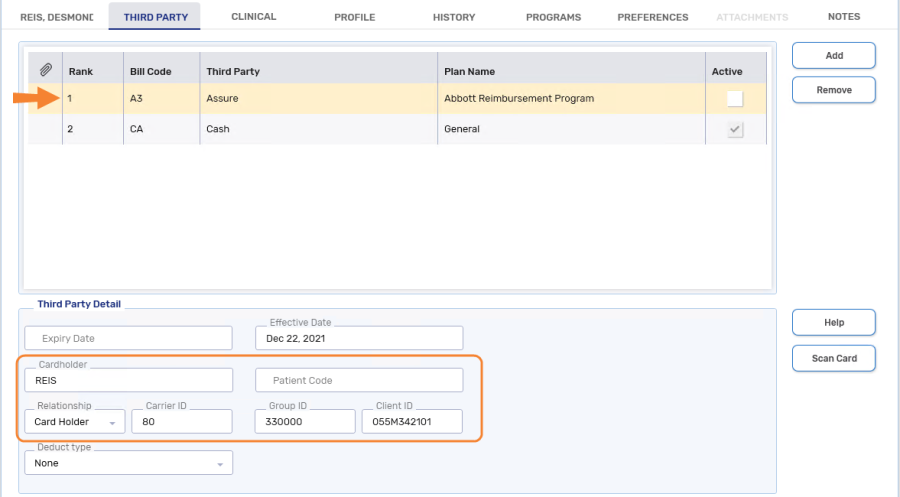
-
Bill Code = A3 (Assure - Abbott Reimbursement Program)
Ensure the Active checkbox is OFF (unchecked). When a plan is inactive, it can be used to bill for the reimbursement program and won't be used in other prescriptions.
-
Cardholder = The first 5 characters of the patient's last name (entering the patient's complete last name is also acceptable)
-
Relationship = Card Holder
-
Carrier ID = 80
-
Group ID = 330000
-
Client ID = enter the last 8 digits of the serial number from the warranty card followed by 01 (e.g. 055M3421 should now read 055M342101).
All meters will have 12 digits in the serial number. Use ONLY the LAST 8 digits of the serial number, excluding all dashes and spaces; any letters must be in uppercase (i.e. CEMU055-M3421 must be entered as 055M3421).
Related Topics
Submitting a Claim for the Abbott Reimbursement Program
To submit a claim for the reimbursement program:
-
From the Workbench or the patient's Profile tab, create a new prescription for the patient using the following information:
-
Enter the Prescriber.
-
Enter the Drug Name
-
Qty Auth = 1 for a meter or the appropriate quantity for lancets
-
Qty = 1 for a meter or the appropriate quantity for lancets
-
SIG = TEST AS DIRECTED BY PHYSICIAN
-
DS = 1 for a meter or the appropriate quantity for lancets
-
-
Select Process. The prescription opens in Rx Detail.
-
Enter A3/CA in the Bill field.
If you are in a province that requires a government plan as the first payer for DUR purposes, ensure it is entered in the Bill field in front of A3/CA (e.g. in British Columbia the bill code would be PC/A3/CA).
-
Verify the pricing matches the total reimbursement amount for the meter or lancet. The total reimbursement amount should be entered as a cost with no markup or fee. Verify the remaining information in Rx Detail and make any necessary changes.
-
Select the Third Party tab.
-
For the A3 portion of the claim, ensure the appropriate Telus PIN is entered in the Alternative DIN field.
For a list of Telus PINs for each blood glucose meter, see the Telus Health Pharmacy Manual.
-
Continue to process the prescription as usual.
Ensure all required supporting documentation is scanned and attached to the prescription for record keeping and audit purposes.
Auto Control Medical Reimbursement Program
The Auto Control Medical (ACM) Reimbursement Program is a drug plan available to all stores and patients for reimbursement of eligible blood glucose monitoring devices. The plan is adjudicated through TELUS Health Assure.
Auto Control Medical Meter PINs
In Propel Rx, pseudo PINs were entered for each Auto Control meter. To locate these PINs, search by trade name (e.g., GE 200, Bionime GM 100, etc.).
Patient Eligibility
To submit a claim to the reimbursement program for a meter or lancets, the following Third Party information must be added to the patient's Third Party tab.
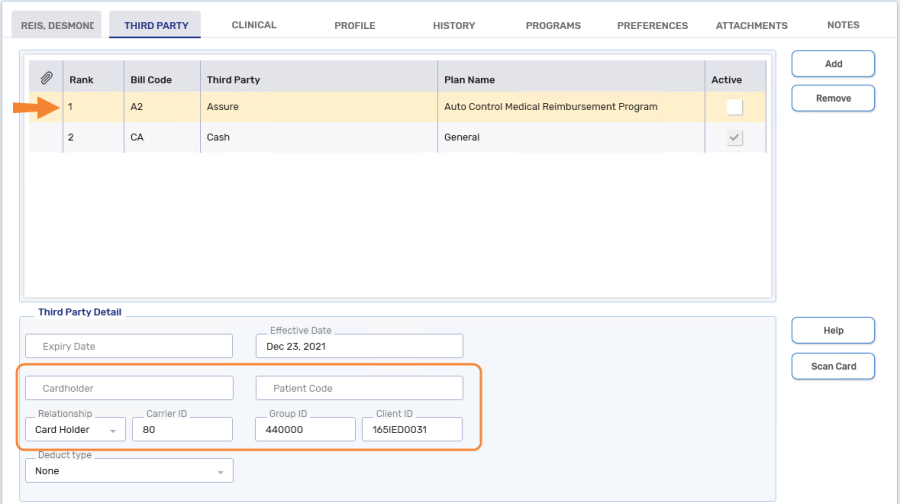
-
Bill Code = A2 (Assure - Auto Control Medical Reimbursement Program)
Ensure the Active checkbox is OFF (unchecked). When a plan is inactive, it can be used to bill for the reimbursement program and won't be used in other prescriptions.
-
Cardholder = The first 5 characters of the patient's last name (entering the patient's complete last name is also acceptable)
-
Relationship = Card Holder
-
Carrier ID = 80
-
Group ID = 440000
-
Client ID = enter the last 7 digits of the serial number from the warranty card followed by 01
When entering the serial number, exclude all dashes and spaces; any letters must be in uppercase (e.g. 165ied0031 would be entered as IED003101).
Related Topics
Submitting a Claim for the ACM Reimbursement Program
To submit a claim for the reimbursement program:
-
From the Workbench or the patient's Profile tab, create a new prescription for the patient using the following information:
-
Enter the Prescriber.
-
Enter the Drug Name
-
Qty Auth = 1
-
Qty = 1
-
SIG = TEST AS DIRECTED BY PHYSICIAN
-
DS = 1
-
-
Select Process. The prescription opens in Rx Detail.
-
Enter A2/CA in the Bill field.
If you are in a province that requires a government plan as the first payer for DUR purposes, ensure it is entered in the Bill field in front of A2/CA (e.g. in British Columbia the bill code would be PC/A2/CA).
-
Verify the pricing matches the total reimbursement amount for the meter. The total reimbursement amount should be entered as a cost with no markup or fee. Verify the remaining information in Rx Detail and make any necessary changes.
-
For the A2 portion of the claim, ensure the appropriate Telus PIN is entered in the Alternative DIN field.
For a list of Telus PINs for each blood glucose meter, see the Telus Health Pharmacy Manual.
-
Continue to process the prescription as usual.
Ensure all required supporting documentation is scanned and attached to the prescription for record keeping and audit purposes.
Ascensia Reimbursement Program
The Ascensia Meters Reimbursement Program is a drug plan available to all stores and patients for reimbursement of eligible blood glucose monitoring devices. The plan is adjudicated through TELUS Health Assure.
Ascensia PINs
In Propel Rx, pseudo PINs were entered for each Ascensia meter. To locate these PINs, search by trade name (e.g., Contour Next EZ Meter, Contour Next USB Meter, etc.).
Patient Eligibility
To submit a claim to the reimbursement program for a meter, the following Third Party information must be added to the patient's Third Party tab.
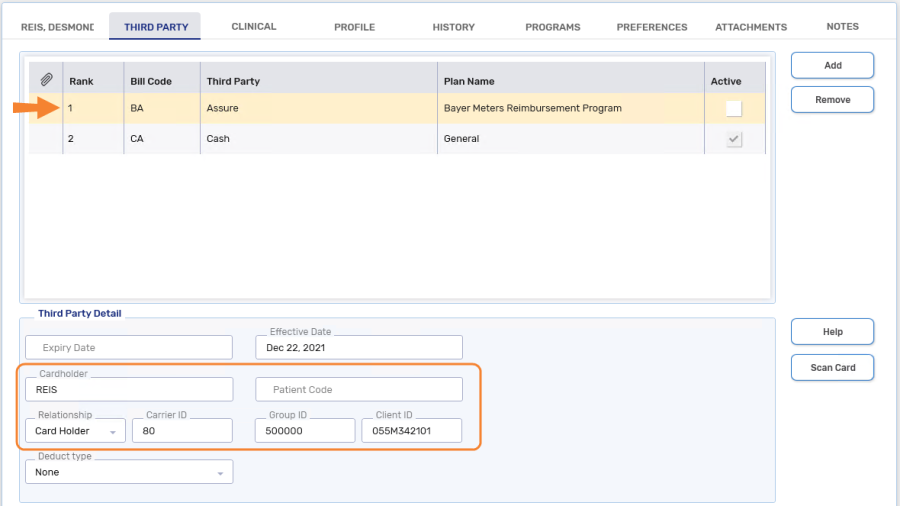
-
Bill Code = BA (Assure - Bayer Meters Reimbursement Program)
Ensure the Active checkbox is OFF (unchecked). When a plan is inactive, it can be used to bill for the reimbursement program and won't be used in other prescriptions.
-
Cardholder = The first 5 characters of the patient's last name (entering the patient's complete last name is also acceptable)
-
Relationship = Card Holder
-
Carrier ID = 80
-
Group ID = 500000
-
Client ID = enter the serial number from the warranty card followed by 01 (e.g. 55M32691421 should now read 55M3269142101). Any letters must be in uppercase. Omit all dashes and spaces.
Related Topics
Submitting a Claim for the Ascensia Meters Reimbursement Program
To submit a claim for the reimbursement program:
-
From the Workbench or the patient's Profile tab, create a new prescription for the patient using the following information:
-
Enter the Prescriber.
-
Enter the Drug Name
-
Qty Auth = 1
-
Qty = 1
-
SIG = TEST AS DIRECTED BY PHYSICIAN
-
DS = 1
-
-
Select Process. The prescription opens in Rx Detail.
-
Enter BA/CA in the Bill field.
If you are in a province that requires a government plan as the first payer for DUR purposes, ensure it is entered in the Bill field in front of BA/CA (e.g. in British Columbia the bill code would be PC/BA/CA).
-
Verify the pricing matches the total reimbursement amount for the meter. The total reimbursement amount should be entered as a cost with no markup or fee. Verify the remaining information in Rx Detail and make any necessary changes.
-
For the BA portion of the claim, ensure the appropriate Telus PIN is entered in the Alternative DIN field.
For a list of Telus PINs for each blood glucose meter, see the Telus Health Pharmacy Manual.
-
Continue to process the prescription as usual.
Ensure all required supporting documentation is scanned and attached to the prescription for record keeping and audit purposes.
Lifescan Meter Reimbursement Program
The Lifescan Meter Reimbursement Program is a drug plan available to all stores and patients for reimbursement of eligible blood glucose monitoring devices. The plan is adjudicated through TELUS Health Assure.
Lifescan Meter PINs
In Propel Rx, pseudo PINs were entered for each Lifescan meter. To locate these PINs, search by trade name (e.g., OneTouch Verio Flex, OneTouch Ultra, etc.).
Patient Eligibility
To submit a claim to the reimbursement program for a meter, the following Third Party information must be added to the patient's Third Party tab.
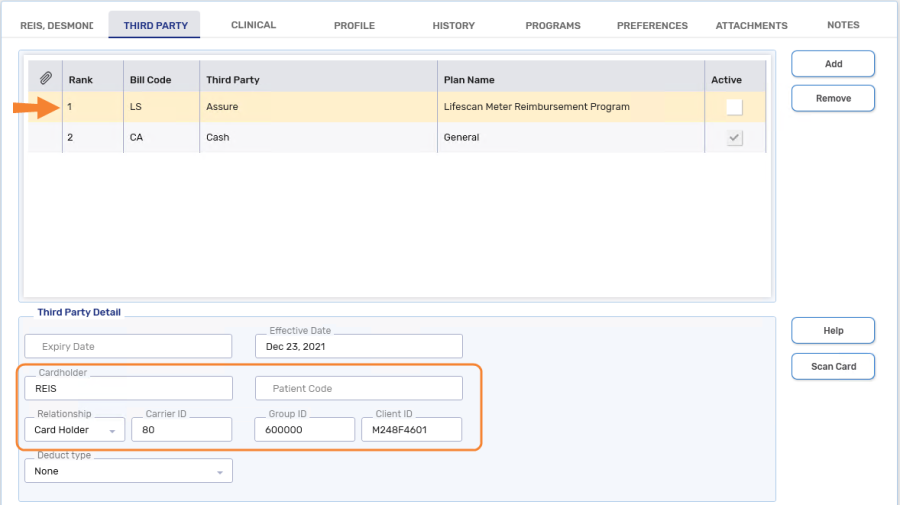
-
Bill Code = LS (Assure - Lifescan Meter Reimbursement Program)
Ensure the Active checkbox is OFF (unchecked). When a plan is inactive, it can be used to bill for the reimbursement program and won't be used in other prescriptions.
-
Cardholder = The first 5 characters of the patient's last name (entering the patient's complete last name is also acceptable)
-
Relationship = Card Holder
-
Carrier ID = 80
-
Group ID = 600000
-
Client ID = enter the serial number from the back or side of the meter followed by 01 (e.g. M248F46 should now read M248F4601).
When entering the serial number, exclude all dashes and spaces; any letters must be in uppercase (e.g. m248f46 would be entered as M248F46).
Related Topics
Submitting a Claim for the Lifescan Meters Reimbursement Program
To submit a claim for the reimbursement program:
-
From the Workbench or the patient's Profile tab, create a new prescription for the patient using the following information:
-
Enter the Prescriber.
-
Enter the Drug Name
-
Qty Auth = 1
-
Qty = 1
-
SIG = TEST AS DIRECTED BY PHYSICIAN
-
DS = 1
-
-
Select Process. The prescription opens in Rx Detail.
-
Enter LS/CA in the Bill field.
If you are in a province that requires a government plan as the first payer for DUR purposes, ensure it is entered in the Bill field in front of LS/CA (e.g. in British Columbia the bill code would be PC/LS/CA).
-
Verify the pricing matches the total reimbursement amount for the meter. The total reimbursement amount should be entered as a cost with no markup or fee. Verify the remaining information in Rx Detail and make any necessary changes.
-
For the LS portion of the claim, ensure the appropriate Telus PIN is entered in the Alternative DIN field.
For a list of Telus PINs for each blood glucose meter, see the Telus Health Pharmacy Manual.
-
Continue to process the prescription as usual.
Ensure all required supporting documentation is scanned and attached to the prescription for record keeping and audit purposes.
Roche Diagnostics Reimbursement Program
The Roche Diagnostics Reimbursement Program is a drug plan available to all stores and patients for reimbursement of eligible blood glucose monitoring devices. The plan is adjudicated through TELUS Health Assure.
Roche Diagnostics Meter PINs
In Propel Rx, pseudo PINs were entered for each Roche diganostics meter. To locate these PINs, search by trade name (e.g., Accu-Chek Aviva, Accu-Chek Compact, etc.).
Patient Eligibility
To submit a claim to the reimbursement program for a meter, the following Third Party information must be added to the patient's Third Party tab.

-
Bill Code = RD (Assure - Roche Diagnostics Program)
Ensure the Active checkbox is OFF (unchecked). When a plan is inactive, it can be used to bill for the reimbursement program and won't be used in other prescriptions.
-
Cardholder = The first 5 characters of the patient's last name (entering the patient's complete last name is also acceptable)
-
Relationship = Card Holder
-
Carrier ID = 80
-
Group ID = 710000
-
Client ID = enter the serial number from the back of the meter followed by 01 (e.g. M248F46 should now read M248F4601).
When entering the serial number, exclude all dashes and spaces; any letters must in uppercase (i.e. m248f46 must be entered as M248F4601
Related Topics
Submitting a Claim for the Roche Diagnostics Reimbursement Program
To submit a claim for the reimbursement program:
-
From the Workbench or the patient's Profile tab, create a new prescription for the patient using the following information:
-
Enter the Prescriber.
-
Enter the Drug Name
-
Qty Auth = 1
-
Qty = 1
-
SIG = TEST AS DIRECTED BY PHYSICIAN
-
DS = 1
-
-
Select Process. The prescription opens in Rx Detail.
-
Enter RD/CA in the Bill field.
If you are in a province that requires a government plan as the first payer for DUR purposes, ensure it is entered in the Bill field in front of RD/CA (e.g. in British Columbia the bill code would be PC/RD/CA).
-
Verify the pricing matches the total reimbursement amount for the meter. The total reimbursement amount should be entered as a cost with no markup or fee. Verify the remaining information in Rx Detail and make any necessary changes.
-
For the RD portion of the claim, ensure the appropriate Telus PIN is entered in the Alternative DIN field.
For a list of Telus PINs for each blood glucose meter, see the Telus Health Pharmacy Manual.
-
Continue to process the prescription as usual.
Ensure all required supporting documentation is scanned and attached to the prescription for record keeping and audit purposes.